by John Walsh, P.A., C.D.E., Ruth Roberts, M.A.
Eye Complications | Changes At Diagnosis | Background Retinopathy | Preproliferative Retinopathy | Proliferative Retinopathy | Macular Edema | Cataracts | Why Damage Occurs
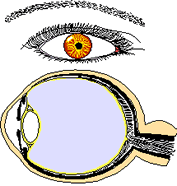
Damage to the eye is the most feared complication of diabetes. And no wonder: the eye is the one-inch spherical marvel that gives us vision. Our vision is created when light reflects from things in our field of vision, gets focused by the cornea and lens, then travels through the transparent gel in the middle of the eye and triggers sensory nerves in the retina.
The retina itself is an ultrathin layer of blood vessels and nerve endings called rods and cones, on the inner back wall of the eye. Signals activated by light in the retina travel to the brain cortex where a three-dimensional picture is given to the outside world. Vision lets us read, drive, and recognize faces, permits manufacturing and microscopy, and enables astronomy from ancient photons that left faraway stars millions of years ago.
Total blindness in diabetes is uncommon since just under 2% of people with IDDM actually suffer total vision loss. However, the fear of losing one’s sight is strong, as anyone with diabetes who’s had a change in vision can testify. This fear can be used to promote self-care, but instead often interferes with taking the steps necessary to avoid vision loss. Diabetes is the most common cause of blindness in the U.S. among younger individuals, although most of this loss can be avoided with better control and through early detection of eye damage.
This article details various types of eye damage found in diabetes, some of the mechanisms involved, and how each is detected. In later columns, we’ll discuss proven therapies like laser photocoagulation, and also potential biochemical interventions that might allow different types of eye damage to be prevented or reversed. Preventing eye damage has been demonstrated in several research studies, particularly the DCCT, where retinopathy was reduced by as much as 76% through improved blood sugar control. However, the reversal of existing eye damage has not yet been documented, although follow-up of individual cases over a number of years certainly suggests some reversal is occurring.
Unless an eye exam is done, most people are unaware that they have eye damage. In one statewide survey in Wisconsin, 23% of people with IDDM and 10% of people with NIDDM on insulin already had proliferative retinopathy, described below. Many were unaware they had these severe eye changes.
Retina damage is usually discovered during a routine exam of the retina. Anyone who’s had IDDM for 5 years or more and everyone with NIDDM should have this detailed eye exam done at least yearly or as recommended by your physician.
Take a look at these great resources on eye care and diabetic retinopathy:
