 Understanding the types of diabetes is one of the most important things you can do after a diagnosis — because not all diabetes is the same, and the type you have determines how it behaves, what treatment you need, and what your long-term outlook looks like. While Type 1 and Type 2 are the most familiar, there are several other forms, including LADA (sometimes called Type 1.5), gestational diabetes, and rarer genetic types. A misdiagnosis — especially mistaking LADA for Type 2 — can delay the right treatment and lead to avoidable complications.
Understanding the types of diabetes is one of the most important things you can do after a diagnosis — because not all diabetes is the same, and the type you have determines how it behaves, what treatment you need, and what your long-term outlook looks like. While Type 1 and Type 2 are the most familiar, there are several other forms, including LADA (sometimes called Type 1.5), gestational diabetes, and rarer genetic types. A misdiagnosis — especially mistaking LADA for Type 2 — can delay the right treatment and lead to avoidable complications.
This guide explains each major type in plain language, with a side-by-side comparison and guidance on what tests to ask for if something about your diagnosis does not seem to fit. All information reflects the ADA Standards of Care 2026 and the CDC’s latest national statistics.
Jump to: Frequently Asked Questions ↓
What Are the Different Types of Diabetes? A Side-by-Side Comparison
The tables below provide a quick overview of the main types of diabetes. Use them to get oriented, then read each section for the full picture.
Clinical overview
| Type | Primary Cause | Typical Age at Onset | Insulin Required? |
|---|---|---|---|
| Type 1 | Autoimmune attack on beta cells | Any age; often childhood or young adult | Always |
| LADA (Type 1.5) | Slow autoimmune process | Typically adults 30+ | Eventually |
| Type 2 | Insulin resistance + declining production | Adults; increasingly teens | Sometimes |
| Gestational | Pregnancy hormones cause insulin resistance | During pregnancy only | Sometimes, temporarily |
| MODY | Single gene mutation | Teens and young adults | Rarely |
| CFRD | Cystic fibrosis–related pancreatic damage | People with CF, any age | Yes |
Diagnostic overview
| Type | Autoantibodies Present? | Key Diagnostic Tests | Important Note |
|---|---|---|---|
| Type 1 | Yes (GAD65, IA-2, ZnT8) | Autoantibody panel, C-peptide, A1c | Run antibody tests before starting insulin if possible |
| LADA (Type 1.5) | Yes (especially GAD65) | GAD65, IA-2, C-peptide | Often misdiagnosed as Type 2 in adults |
| Type 2 | Rarely | A1c, fasting glucose, C-peptide | C-peptide typically normal or high early on |
| Gestational | No | Oral glucose tolerance test | Screening recommended weeks 24–28 of pregnancy |
| MODY | No | Genetic testing | Requires specialist referral for genetic panel |
| CFRD | No | Annual 2-hr OGTT from age 10 (CFF guidance) | Standard fasting glucose tests can miss CFRD |
Not sure which type you have? Ask your doctor about a C-peptide test and an autoantibody panel. These tests often help clarify the diagnosis, though interpretation depends on timing and clinical context — they are most reliably run before insulin treatment has begun, since therapy can affect results. Free screening for relatives of people with Type 1 is available at TrialNet.org.
What Is Diabetes and Why Does Blood Sugar Rise?
Diabetes is a group of conditions in which the body cannot properly manage blood sugar (glucose). Normally, the pancreas releases a hormone called insulin to move glucose from the bloodstream into your cells for energy. With diabetes, this process breaks down — either because the pancreas produces little or no insulin, or because the body’s cells do not respond to insulin properly, or both.
When glucose cannot enter cells, it builds up in the bloodstream. Over time, persistently high blood sugar damages blood vessels and nerves throughout the body, increasing the risk of complications affecting the eyes, kidneys, heart, and feet. The encouraging news is that keeping your blood sugar in a healthy range — through medication, food choices, activity, and monitoring — dramatically reduces these risks. About 1 in 8 Americans now lives with diabetes, and understanding your specific type is the first step to managing it well.
What Is Type 1 Diabetes?
Type 1 diabetes is an autoimmune disease. The immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas, eventually leaving the body with little or no ability to produce insulin. It is not caused by diet or lifestyle. People with Type 1 require insulin to survive, beginning at diagnosis and continuing for life. According to the CDC’s January 2026 National Diabetes Statistics Report, over 2 million Americans are living with Type 1 diabetes, including approximately 314,000 children and adolescents.
Type 1 can develop at any age, though it is most commonly diagnosed in children, teenagers, and young adults. Adult-onset Type 1 is more common than previously thought — research suggests that roughly 42% of new Type 1 diagnoses occur in people over age 30, which is one reason it is sometimes misdiagnosed as Type 2 in adults.
What are the symptoms of Type 1 diabetes?
Symptoms often come on suddenly and can include:
- Frequent urination (especially at night)
- Excessive thirst
- Unexplained weight loss
- Extreme fatigue
- Blurred vision
- Fruity-smelling breath (a sign of diabetic ketoacidosis, or DKA — a medical emergency)
How is Type 1 diabetes diagnosed and treated?
Diagnosis involves autoantibody testing (looking for GAD65, IA-2, and ZnT8 antibodies) and a C-peptide test. A very low or undetectable C-peptide supports severe insulin deficiency consistent with Type 1 diabetes, especially in the right clinical setting — though C-peptide can still be measurable early in the disease during a “honeymoon phase,” which is one reason clinical context matters alongside test results. An A1c test assesses average blood sugar levels over 2–3 months. Treatment requires daily insulin, delivered by injection or an insulin pump or automated insulin delivery (AID) system. Many people with Type 1 now use continuous glucose monitors (CGMs) paired with AID systems, which adjust insulin doses automatically in real time.
Teplizumab (Tzield) is the first FDA-approved disease-modifying therapy for autoimmune Type 1 diabetes. It is currently approved for people aged 8 and older with Stage 2 T1D — confirmed autoantibodies plus abnormal blood sugar before clinical symptoms begin — to delay the onset of clinical Type 1 diabetes. Additional indications are under regulatory review. For the most current information, ask your endocrinologist or visit TrialNet.org for screening and clinical trial options.
What Is LADA (Type 1.5 Diabetes)?
LADA — Latent Autoimmune Diabetes in Adults — is not a formal ADA diagnostic category, but a commonly used clinical term for a form of autoimmune diabetes that shares features of both Type 1 and Type 2. Like Type 1, it involves an autoimmune attack on insulin-producing beta cells. Unlike Type 1, the process is slower, unfolding over months or years rather than weeks. This means people with LADA often appear to manage well on oral medications at first, before eventually requiring insulin as their beta cells decline further. (You may also see it referred to as Type 1.5 in some sources.)
LADA is typically seen in adults over age 30, and people who have it are often not overweight, which can make it look less like “typical” Type 2 diabetes. Researchers estimate that between 5–10% of people currently diagnosed with Type 2 may actually have LADA.
Why does a LADA misdiagnosis matter?
Certain medications commonly prescribed for Type 2 — particularly sulfonylureas, which push the pancreas to produce more insulin — have been associated with faster loss of beta-cell function in LADA and are generally not preferred. Starting insulin earlier, once autoantibodies are confirmed, may help preserve remaining beta-cell function longer. The most important diagnostic test is a GAD65 autoantibody measurement, which is positive in the vast majority of LADA cases. If you were diagnosed with Type 2 as an adult, are not overweight, and are finding that oral medications are not controlling your blood sugar well, ask your doctor about LADA testing. Note that autoantibody tests are most reliably interpreted before insulin treatment has begun.
What Is Type 2 Diabetes?
Type 2 diabetes is the most common form, accounting for 90–95% of all diabetes cases. It develops when the body becomes resistant to insulin — meaning cells do not respond to it effectively — and the pancreas gradually loses the ability to compensate by producing more. Blood sugar rises as a result. According to CDC 2026 data, approximately 38 million Americans have Type 2 diabetes.
Type 2 is strongly associated with lifestyle and metabolic factors, though genetics also play a meaningful role. It is no longer a condition that only affects older adults: rates among children and teenagers have increased significantly over the past two decades, particularly in certain racial and ethnic groups.
What are the risk factors for Type 2 diabetes?
- Overweight or obesity (especially excess abdominal fat)
- Physical inactivity
- Family history of Type 2 diabetes in a parent or sibling
- Age 45 or older (though younger cases are increasing)
- Certain ethnic backgrounds: African American, Hispanic/Latino, American Indian, Alaska Native, Asian American, and Pacific Islander populations face a higher risk
- History of gestational diabetes or delivering a baby weighing more than 9 pounds
- Prediabetes: a fasting blood sugar of 100–125 mg/dL (5.6–6.9 mmol/L) or an A1c of 5.7–6.4%
How is Type 2 diabetes treated?
Treatment often starts with lifestyle changes (diet, exercise, and weight management) alongside medication. Metformin remains a common first-line medication. GLP-1 receptor agonists such as semaglutide (Ozempic, Wegovy) are now widely used and have demonstrated benefits for blood sugar, body weight, and cardiovascular risk. Tirzepatide (Mounjaro, Zepbound) is a dual GIP/GLP-1 receptor agonist — a distinct but related drug class, now formally categorized separately in the ADA 2026 Standards of Care — with similarly strong clinical results. As the condition progresses, insulin may eventually be needed.
On monitoring: the ADA 2026 Standards recommend considering CGM at diabetes onset and at any time thereafter for people who could benefit from continuous monitoring, including those not using insulin. This is a guideline recommendation based on growing evidence of benefit across diabetes types. Insurance coverage is a separate question: Medicare currently covers CGMs primarily for people who use insulin or have a history of problematic low blood sugar. If you are managing Type 2 with oral medications only, check your specific plan, as commercial coverage varies.
What Is Gestational Diabetes?

Gestational diabetes typically resolves after delivery, but it carries real risks: a higher likelihood of a large baby (macrosomia), delivery complications, and preeclampsia. NIDDK notes that about half of women with gestational diabetes go on to develop Type 2 diabetes, often within 5 to 10 years. Blood sugar should continue to be monitored after pregnancy. Treatment focuses on blood sugar monitoring, dietary changes, physical activity, and insulin or oral medications if needed.
What Are the Other Specific Types of Diabetes?
Beyond the four main types, several less common forms of diabetes arise from genetic mutations, other medical conditions, or medications.
MODY — Maturity-Onset Diabetes of the Young
MODY is caused by mutations in a single gene that regulates insulin production or secretion. It accounts for roughly 1–2% of all diabetes cases but is frequently misdiagnosed as either Type 1 or Type 2. People with MODY are often diagnosed before age 25, are rarely overweight, and typically have a strong family history of diabetes across multiple generations. Because MODY is caused by a specific genetic defect, the right treatment depends on which gene is involved — some forms respond well to sulfonylureas, others do not require insulin at all. Genetic testing is required for a definitive MODY diagnosis.
CFRD — Cystic Fibrosis–Related Diabetes
CFRD affects people with cystic fibrosis as the disease progressively damages the pancreas, impairing both insulin production and release. It shares features of both Type 1 (insulin deficiency) and Type 2 (some insulin resistance), making it a uniquely complex condition. The Cystic Fibrosis Foundation (CFF) recommends an annual 2-hour 75g oral glucose tolerance test starting at age 10 for people with CF, as standard fasting glucose tests can miss CFRD. Treatment almost always involves insulin, and management must be carefully coordinated with overall CF care — particularly around nutrition, since caloric needs in CF are often higher than typical diabetes management guidelines assume.
Steroid-Induced Diabetes
Corticosteroids such as prednisone, used to treat inflammatory conditions, organ transplant rejection, and various other diseases, can cause or worsen high blood sugar. In people without underlying diabetes, this is usually temporary and resolves when the steroid is stopped or tapered. In people with existing diabetes or prediabetes, steroids can significantly worsen control and may require medication adjustments. Blood sugar monitoring is important for anyone on extended or high-dose steroid therapy.
Could Your Diabetes Diagnosis Be Wrong?
Misdiagnosis is more common than most people realize, particularly for adult-onset Type 1 and LADA, which are frequently mistaken for Type 2. Getting the correct diagnosis matters — it directly shapes which medications are safe and effective for you.
| Misdiagnosed As | Actually Is | Why It’s a Problem | What to Ask For |
|---|---|---|---|
| Type 2 | LADA (Type 1.5) | Sulfonylureas are associated with faster beta-cell loss; insulin is needed sooner | GAD65 autoantibody test, C-peptide |
| Type 2 | Type 1 (adult onset) | Insulin delay increases DKA risk and leads to poor control | Full autoantibody panel (GAD65, IA-2, ZnT8), C-peptide |
| Type 1 or 2 | MODY | Wrong medication class; some MODY types respond to sulfonylureas, not insulin | Genetic testing (request endocrinologist referral) |
Tests worth asking your provider about: Autoantibody testing (GAD65 first; if negative, follow with IA-2 and ZnT8 per ADA 2026 guidance), a C-peptide test (measures remaining insulin production), and genetic testing if MODY is suspected. These tests often help clarify the diagnosis, though interpretation depends on timing and clinical context — autoantibody tests are most reliably interpreted before insulin treatment has begun, since therapy can complicate results. Free screening for relatives of people with Type 1 is available through TrialNet.org.
What Technology and Tools Are Available for All Diabetes Types?
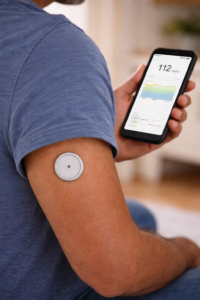
- Continuous glucose monitors (CGMs): CGMs track your blood sugar automatically every few minutes. The ADA 2026 Standards recommend considering CGM for anyone who could benefit, including people not using insulin. Coverage varies — Medicare ties CGM coverage primarily to insulin use or a history of low blood sugar episodes, while commercial plans differ. Check with your insurer.
- Automated insulin delivery (AID) systems: AID systems pair a CGM with a smart insulin pump that adjusts doses automatically. The ADA 2026 Standards removed prior prerequisites for AID initiation, streamlining access to this technology.
- Smart insulin pens: Connected injection pens that track dose timing and amounts, helping people on multiple daily injections manage their regimen more accurately.
- Mobile apps: Apps for carb tracking, insulin dose calculation, blood sugar logging, and trend analysis are widely available and increasingly integrated with CGM and pump data.
Helpful Resources and Research
- ADA Standards of Care in Diabetes — 2026 (Section 2: Diagnosis and Classification of Diabetes)
- CDC National Diabetes Statistics Report, January 2026
- NIDDK — Gestational Diabetes
- TrialNet — Free T1D Screening for Relatives
- Cystic Fibrosis Foundation — CFRD Guidelines
- NIDDK — Diabetes Overview
Frequently Asked Questions
What is the most common type of diabetes?
Type 2 diabetes is by far the most common, accounting for 90–95% of all diabetes cases. Approximately 38 million Americans have Type 2 diabetes per CDC 2026 data. Type 1 affects over 2 million Americans, with other types — LADA, MODY, gestational, and CFRD — making up the remainder.
What is the difference between Type 1 and Type 2 diabetes?
Type 1 is an autoimmune disease in which the immune system destroys insulin-producing cells, requiring daily insulin from diagnosis onward — it is not preventable. Type 2 involves insulin resistance, where the body still produces insulin but cannot use it effectively, and is often managed with lifestyle changes and oral medications before insulin is needed. Type 1 can occur at any age; Type 2 is more common in adults but increasingly seen in younger people.
Can you have diabetes without knowing it?
Yes — the CDC estimates that about 1 in 4 adults with diabetes in the U.S. are undiagnosed, approximately 11 million people. Type 2 can develop gradually with few noticeable symptoms for years. Regular screening is recommended for adults 35 and older, and earlier for anyone with risk factors such as overweight, family history, or prediabetes.
Is LADA the same as Type 1 diabetes?
LADA (Latent Autoimmune Diabetes in Adults) is a form of autoimmune diabetes biologically similar to Type 1 but progressing more slowly — people typically retain some insulin production for years before needing insulin. It is not a formal ADA diagnostic category, but a widely used clinical term. Because of its slower progression, LADA is frequently mistaken for Type 2 when it first appears in adults.
What blood sugar level is too high?
For most non-pregnant adults, the ADA recommends blood sugar between 80–130 mg/dL (4.4–7.2 mmol/L) before meals and below 180 mg/dL (10.0 mmol/L) two hours after eating. Blood sugar consistently above these levels increases the risk of long-term complications affecting the eyes, kidneys, heart, and nerves. A single reading of 200 mg/dL (11.1 mmol/L) or higher with symptoms is one of the diagnostic criteria for diabetes.
Can Type 2 diabetes go into remission?
Yes — some people with Type 2 diabetes can achieve remission, meaning blood sugar returns to a normal range without medication, most often through significant weight loss (typically 10–15% or more of body weight). The ADA uses the term “remission” rather than “reversal” because the underlying susceptibility remains and blood sugar should continue to be monitored. Type 1 and LADA cannot go into remission.
What tests confirm which type of diabetes I have?
The most useful tests are an autoantibody panel (starting with GAD65, followed by IA-2 and ZnT8 if negative) and a C-peptide test, which measures how much insulin the pancreas is still producing. These tests often help clarify the diagnosis, though they are most reliably interpreted before insulin treatment has started. If MODY is suspected, genetic testing is required — a standard A1c or fasting glucose test cannot distinguish between diabetes types.
Does gestational diabetes mean my baby will have diabetes?
Having gestational diabetes does not mean your baby will be born with diabetes, but it does slightly increase the child’s long-term risk of obesity and Type 2 diabetes. The more immediate concern is the risk of a larger-than-average baby (macrosomia), which can complicate delivery. With proper management — blood sugar monitoring, dietary changes, and medication when needed — most women with gestational diabetes have healthy pregnancies and babies.
What is the newest treatment for Type 1 diabetes?
Teplizumab (Tzield) is the first FDA-approved disease-modifying therapy for autoimmune Type 1 diabetes, currently approved for people aged 8 and older with Stage 2 T1D to delay the onset of clinical disease. Additional indications are under regulatory review. For people already living with Type 1, automated insulin delivery (AID) systems — pairing a CGM with a smart insulin pump — represent the most significant advance in day-to-day management in recent years.
How do I know if my diabetes diagnosis is correct?
If you were diagnosed with Type 2 as an adult but are not overweight, have a personal or family history suggesting autoimmune diabetes, or are not responding well to oral medications, it is worth asking your doctor about LADA — starting with a GAD65 autoantibody test and C-peptide, ideally before starting insulin. If MODY is a possibility based on young age of diagnosis and strong multi-generational family history, request a referral to an endocrinologist to discuss genetic testing. A second opinion from an endocrinologist is always a reasonable step if you have doubts about your diagnosis.
Last Updated on April 16, 2026
