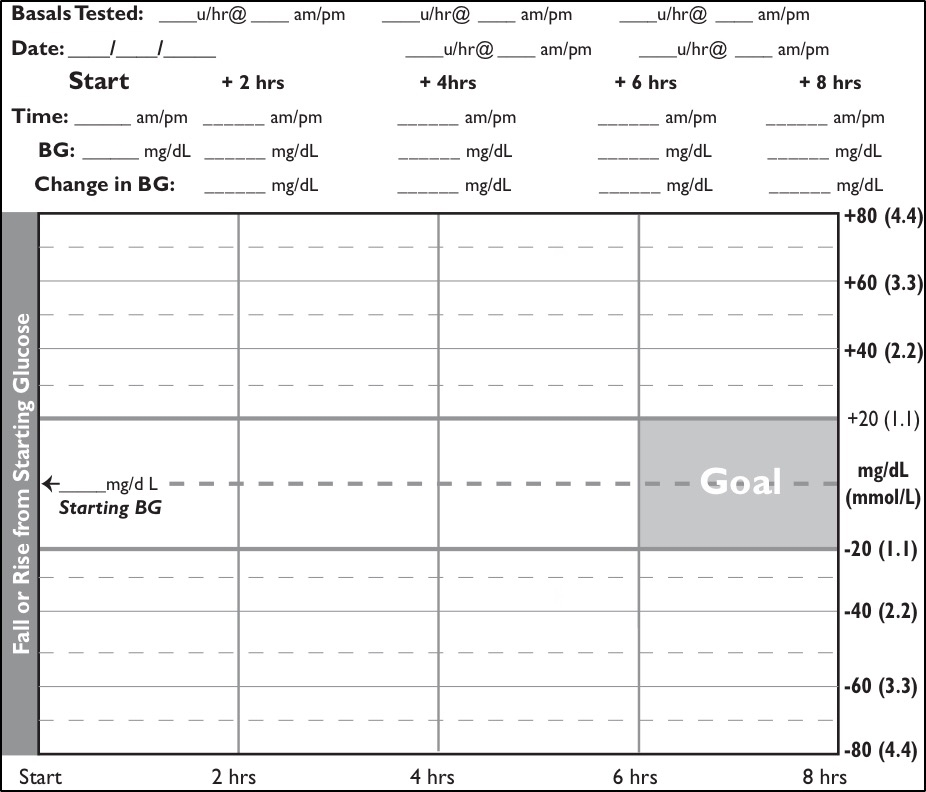
Download and print out this Basal/LAI Checking Tool derived from Pumping Insulin, and use it to graph the results and adjust your Basal Rates or LAI. Be sure to compare your settings with those of pump wearers in excellent control in the right column of the Pump Settings Tool.
Basal insulin from a pump or a LAI delivers roughly half of the day’s total insulin as a steady release around the clock. This insulin compensates for the liver’s production and the muscles’ release of glucose when you are fasting. Basal insulin helps this glucose enter cells for fuel, rather than backing up and rising in the blood. On MDI, an injection of long-acting insulin each day serves the same function.
Basal rates and LAI are essential because:
- This background insulin provides the foundation for bolus and short-acting insulin doses. Your carb factor and correction factor work more consistently and accurately after your glucose stays steady and level form a constant infusion of background insulin.
- You will need larger meal boluses and larger correction doses for the high readings that result from low basal rates or insufficient LAI. On the other hand, you need smaller meal boluses or extra carbs for lows caused by high basal rates or excessive LAI. Both result in erratic glucose readings.
- Accurate basal rates and lAI doses allow you to skip or delay meals without going low or high. The right amount keeps you sailing smoothly on a steady breeze throughout the day.
Select and Verify Your Basal Rate(s)
Determine your TDD first. Correct basal rates depend on an accurate TDD. If your A1c is higher than 7.5% or 8.0% with few lows, you can find more accurate basal rates and pump settings in the right column of the Pump Settings Tool.
Basal or long-acting insulin typically makes up 40-60% of the total daily dose (TDD) of insulin for adults. Before puberty, athletes, and the thin elderly basal rates may be closer to 40% of the TDD. Selecting a starting basal rate, and then checking and adjusting it provides the best rate(s). You may want to try a single starting basal rate for the entire day and vary that rate based on basal testing.
Most people see their glucose improve when they use 55-60% of the TDD as basal and deliver slightly more during the daytime hours. This reduces post-meal glucose spikes but should not be so excessive that it causes lows.
Basics
Verify your basal rates with three 8-hour intervals of fasting spread throughout the day. Check overnight rates first because they are the easiest to verify, and once adjusted, provide an excellent guide to the selection of daytime basal rates. Sleep accounts for about a third of your life, so having good glucose readings through the night automatically leads to a better A1c, avoids scary lows during the night, and sets you up for better glucose readings through the rest of the day.
If a single basal rate works successfully through the night, start with that for your daytime rate. If you use more than one rate overnight, begin with an average of these rates as your daytime rate.
Split daytime checks into two 8-hour segments done on different days. These shorter periods avoids long periods of fasting that can increase your insulin sensitivity and make your basal requirement appear to be artificially low.
- Check the first half of your day when you can skip breakfast and have a late lunch.
- Check the second half of the day 5 hours or more after your breakfast bolus and 3 hours or more after your last meal. Skip lunch and eat a late dinner once checking is complete.
Before starting to check and adjust your basal rates, be sure to save your current basal rates. Write them down, take a photo of them, or duplicate your basal rates as an alternate basal profile in your pump and adjust these.
Steps to Check Your Basal Rates
On a CGM, temporarily set the high and low alerts at 20 to 25 mg/dl (1.1 mmol/L) above and below your starting glucose. The CGM will then alert you any time your glucose strays. An alternate method for overnight basal checks is to view the 12-hour screen on your CGM in the morning for a few days. Then plot out the glucose trend line for a 6 to an 8-hour period that starts at least 5 hours after your last bolus and last food intake the night before.
On a glucose meter, check your glucose 5 hours after your last bolus, then every 2 hours, or if low glucose symptoms occur.
Basal Checking Tool
- Start a basal check any time your glucose is between 90 and 140 mg/dL (5.0 – 7.8 mmol/L), you have not eaten in the last 3 hours, and have not taken a bolus in the previous 5 hours.
- Eat no carbs, but small amounts of protein (a few nuts, a slice of cheese, or boiled egg) are OK.
- Check your glucose or view your CGM screen and record the value every 1-2 hours on the graph above to plot how your glucose responds over time. Check also if you feel your glucose is low.
- If your glucose goes below 70 mg/dL (3.9 mmol/L), stop checking and have some carbs.
- If your glucose rises or falls more than 20 mg/dL (1.1 mmol/L), see Table 10.5 for adjusting your basal rates.
Repeat basal rate checks and adjustments until they keep your glucose within (+/-) 20 mg/dL (1.1 mmol/L) of your starting glucose.
Adjust Your Basal Rates From Your Results
When needed, change your basal rates using Table 10.5 as a guide. If you need a significant shift in your basal rates, you may also need to adjust your CarbF and CorrF. Table 10.7 shows how much insulin you will add or remove when you change a basal rate over 6, 8, or 24 hours.
| 11.2 How to Change the CarbF (ICR) | |||
|---|---|---|---|
| When you change a basal rate, it helps to know how many total units the change brings. | |||
| Change in Basal Rate | Total units over 6 hrs | Total units over 8 hrs/strong> | Total units over 24 hrs |
| +/- 0.025 u/hr | +/- 0.15 u | +/- 0.2 u | +/- 0.6 u |
| +/- 0.05 u/hr | 0.3 u | 0.4 u/td> | 1.2 u |
| +/- 0.1 u/hr | 0.6 u | 0.8 u | 2.4 u |
| Basal adjustments of 0.025 and 0.1 u/hr equal 0.6 and 2.4 units over the entire day. For a glucose that falls or rises slightly during a basal test, a basal change of 0.025 or 0.05 u/hr (or 0.2 and 0.4 units over 8 hours) may fix this. | |||
For another way to adjust basal rates, divide the rise or fall over 8 hours by your CorrF. Then divide that by 8 to get the units per hour to increase or decrease your basal rate. Let’s say your glucose rises 60 mg/dL over 8 hours, and your CorrF is 30 mg/dl per unit of insulin. Divide 60 mg/dL by 30 mg/dL/unit and you get 2 units. Divide 2 units by 8 hours, and it gives a maximum basal increase of 0.25 u/hr in basal rates. This is a large change, so a person might raise their basal rate by 0.2 u/hr over the 8 hours and then recheck.
An AID Helps You Select the Right Pump Settings
When wearing an automated insulin delivery device, the frequency and timing of basal reductions become clear. You can then make adjustments in your basal and CarbF settings more easily:
- If your basal rate never or rarely gets suspended, your rates are likely too low, unless your A1c is excellent.
- Frequent basal suspensions suggest the prior rates are too high.
- Frequent basal suspensions before meals or at a particular time of day suggest the prior basal rates are too high or the prior CarbF number is too low.
When you change, your rate is often as important as how much you change it. When you change a basal rate in your pump, it takes more than 4 hours to see its full effect.
Basal rates and insulin work slowly, so make basal adjustments early. Adjust basal rates 5 to 8 hours BEFORE a high or low reading occurs, or 2 to 3 hours before your glucose BEGINS to rise or fall.
Don’t chase your basal’s tail! From the time you change a basal rate, the change does not reach its full impact on your glucose until 4 to 5 hours later. Basal rates do not vary much during the day once you make proper adjustments early. If one basal rate is 0.6 u/hr and another is 1.2 u/hr, you are likely chasing the previous basal’s tail. Raise the 0.6 u/hr rate and lower the 1.2 u/hr rate by equal amounts to bring them closer. Bringing rates closer often brings better results.
Now that your basal rates are correct, it’s time to Check Your Carb Factor.
Last Updated on September 19, 2020

