The satiety index for diabetes is a useful tool that ranks how filling different foods are — and for people managing blood sugar, choosing the right filling foods can significantly impact weight control, snacking habits, and daily glucose levels. Developed in the 1990s by Dr. Susanne Holt and colleagues at the University of Sydney, this index scores foods based on how effectively they reduce hunger after a specific number of calories. Knowing which foods score highest — and how to apply that information wisely — can be a valuable part of your diabetes management strategy.
This guide explains what the satiety index is, which foods have the highest scores, how it relates to blood sugar management, and how to use it with tools like continuous glucose monitors (CGMs) and carb counting. Whether you were recently diagnosed or have been managing diabetes for years, you’ll find practical, science-based tips here.
Looking for a specific answer? Go to the Frequently Asked Questions section for quick information about the satiety index and diabetes.
Quick-Reference: Satiety Index for Diabetes at a Glance
- What it is: A ranking of how filling foods are after equal-calorie portions, compared to white bread (score = 100).
- Why it matters: More filling foods can reduce snacking and support weight management, which helps blood sugar and insulin sensitivity.
- Top-scoring foods: Boiled potatoes (323), fish (225), oatmeal (209), whole fruit (197–202), eggs (150).
- Key limit: A high satiety score does not mean a food is low in carbs or won’t raise your blood sugar.
- Best approach: Combine satiety-focused choices with carb counting, your glucose data, and your care team’s guidance.
What is the satiety index, and how was it created?
The satiety index was developed by Dr. Susanne Holt and her team in the 1990s to answer a simple question: after eating the same number of calories from different foods, which ones keep you feeling full the longest?
To find out, volunteers ate equal-calorie portions, about 240 calories (1,000 kJ), of 38 different foods. Over the next two hours, they periodically rated their hunger and fullness. Researchers also recorded how much participants ate at a later meal. White bread was given a baseline score of 100. Foods with scores above 100 were more filling than white bread calorie-for-calorie; those below 100 were less filling.
The results were eye-opening. Boiled potatoes, often feared by people with diabetes, scored an impressive 323, making them one of the most filling foods tested. Croissants, on the other hand, scored just 47. In general, foods high in fiber, water, and/or protein tend to keep people fuller, longer.
What makes a food more filling?
Research since the original study has helped identify why certain foods are more satisfying than others. Foods tend to score higher on the satiety index when they:
- Having a high water content — water adds volume and weight without increasing calories.
- They are high in protein — protein is the most filling macronutrient.
- Contain soluble fiber — it slows digestion and triggers fullness hormones in the gut.
- Require more chewing — solid foods are usually more satisfying than liquids or soft foods.
- Has lower energy density — fewer calories per gram means you get more food for the same calorie count.
This is why a boiled potato outperforms a croissant by nearly 7 to 1, even though both can have the same number of calories in the tested portion.
Why is satiety important for people with diabetes?
For anyone managing diabetes — whether type 1, type 2, or another form — feeling satisfied after meals is about more than just comfort. It directly impacts important health goals.
Satiety aids in weight management.
Excess weight, especially around the abdomen, decreases your body’s response to insulin. When your cells don’t respond well to insulin, blood sugar levels rise. Losing just 5–10% of body weight can significantly improve blood sugar levels and, for some people with type 2 diabetes, lessen the need for medication. Choosing filling foods helps make it easier to consume fewer calories without feeling deprived.
Satiety can help prevent between-meal spikes.
Grazing — snacking often between meals — is a common cause of high blood sugar throughout the day. If your meals keep you full for several hours, you’re less likely to reach for high-carb snacks. Combining your CGM data with your hunger signals can help identify which meals or foods keep you satisfied and which ones leave you hungry an hour later.
Satiety-focused eating aligns with current guidelines.
The ADA Standards of Care 2026 (Section 5: Facilitating Positive Health Behaviors) highlight flexible, personalized nutrition strategies that promote overall well-being — not just blood sugar control. A diet centered on protein, fiber, vegetables, and whole foods naturally promotes both high satiety and high nutrient quality.
Which foods rank highest on the satiety index?
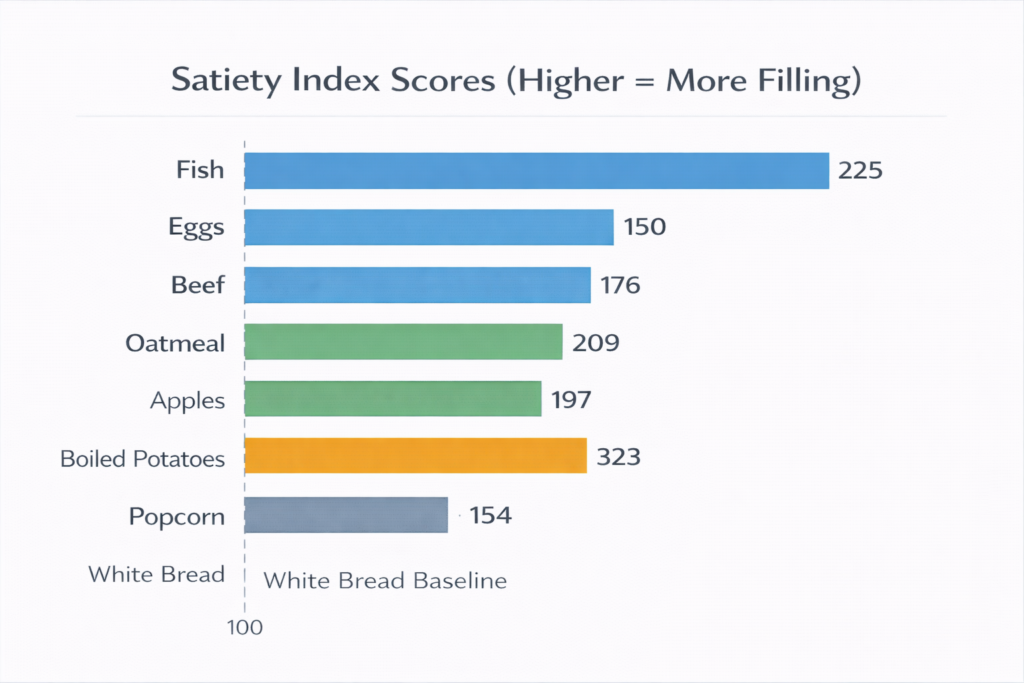
Below are selected foods from the original Holt study, along with context for people with diabetes. All scores are relative to white bread, which is set at 100.
Satiety Index Scores and Blood Sugar Context
| Food | Satiety Score | Carb Level |
|---|---|---|
| Potatoes (boiled) | 323 | High — count carbs |
| Fish | 225 | Very low |
| Oatmeal / porridge | 209 | Moderate — choose less processed |
| Oranges | 202 | Low-moderate |
| Apples | 197 | Low-moderate |
| Brown pasta | 188 | Moderate — watch portion |
| Beef | 176 | Very low |
| Popcorn | 154 | Moderate — watch portion/toppings |
| Eggs | 150 | Negligible |
| White bread | 100 | High — baseline comparison |
| Ice cream | 96 | Moderate + high fat |
| Cake | 65 | High refined carbs and fat |
| Croissant | 47 | High refined carbs and fat |
 How to Incorporate High-Satiety Foods into Diabetes Meal Planning
How to Incorporate High-Satiety Foods into Diabetes Meal Planning
| Food | Best Use for Diabetes | Watch Out For |
|---|---|---|
| Boiled potatoes | Main dish with lean protein | Carb count — portion carefully |
| Fish | High-protein base for any meal | Preparation method (fried adds carbs) |
| Oatmeal | Breakfast with Greek yogurt or eggs | Choose steel-cut; watch toppings |
| Whole fruit | Snack paired with nuts or protein | Juice is far less filling |
| Eggs | Breakfast or snack protein anchor | Watch what you cook them in |
Important note for insulin users: A food with a high satiety score is not necessarily low in carbs. Boiled potatoes are very filling but still contain significant carbohydrates. If you use an insulin pump or take mealtime insulin injections, always base your dose on the carbohydrate content of the meal — not how filling it feels.
How does the satiety index differ from the glycemic index?

- Satiety Index (SI): Measures how full a food makes you feel after equal-calorie portions, focusing on appetite and hunger.
- Glycemic Index (GI): Indicates how fast a food increases your blood sugar relative to pure glucose. Emphasizes the speed of glucose increase.
- Glycemic Load (GL): Combines GI with the actual carbohydrate amount in a serving. Provides a more accurate view of blood sugar effects.
A food can perform well on one scale but not on others. Boiled potatoes are a good example: they have a very high satiety score (323) but also a relatively high GI. That doesn’t make them off-limits for most people with diabetes — it just means portion size and what you pair them with (protein, fat, non-starchy vegetables) matter a lot.
For context: if your pre-meal blood sugar is 120 mg/dL (6.7 mmol/L) and you eat a large portion of boiled potatoes without protein or fat, you’re likely to see a sharp increase — even though you’ll feel quite full afterward. Adding fish or chicken and a green salad will slow the rise in glucose and help you stay satisfied longer.
The best foods for diabetes usually perform well on all three criteria: they are filling, they raise blood sugar gradually, and the total carbohydrate content per serving is manageable. Consider: legumes, non-starchy vegetables, eggs, fish, and whole grains in moderate portions.
What are the limits of the satiety index for people with diabetes?
The satiety index is a really helpful tool — but it has important limitations that are especially crucial for people with diabetes to know.
It was a brief, controlled experiment
The original study tracked hunger and fullness for only two hours, with participants eating one food at a time in a lab setting. Real life is very different: you mix foods at meals, eat under stress, skip sleep, and your hunger hormones change depending on your activity level and medications.
Mixed meals change everything
Adding protein, fat, and fiber to a carbohydrate-rich food slows digestion and helps you feel full longer — and your blood sugar usually rises more gradually as well. The satiety index scores were measured for individual foods eaten alone, so scores can vary significantly in a real meal setting.
Diabetes medications influence hunger and fullness.
If you take GLP-1 medicines like semaglutide or tirzepatide, you might already feel fuller faster because these drugs partly slow down how quickly food leaves your stomach. Other medications, including some insulin regimens, can increase your appetite or lead to cravings after a low. Your personal hunger signals might not align with what the satiety index predicts.
Responses from individuals vary greatly.
Sleep quality, stress levels, exercise, gut health, and conditions like gastroparesis (delayed stomach emptying, more common in long-term diabetes) all influence how full you feel. Two people eating the same high-satiety meal may have very different hunger and blood sugar responses. This is why tracking with a continuous glucose monitor is so useful. It shows your actual blood sugar pattern, not just what the charts predict.
High satiety does not mean low carb.
This can’t be emphasized enough: boiled potatoes are the most filling food in the original study, but a medium boiled potato contains about 30–37 grams of carbohydrate. If you use insulin or a medication that requires carb counting, a high satiety score isn’t a reason to skip your usual carb management practices.
How can you use the satiety index to manage diabetes daily?
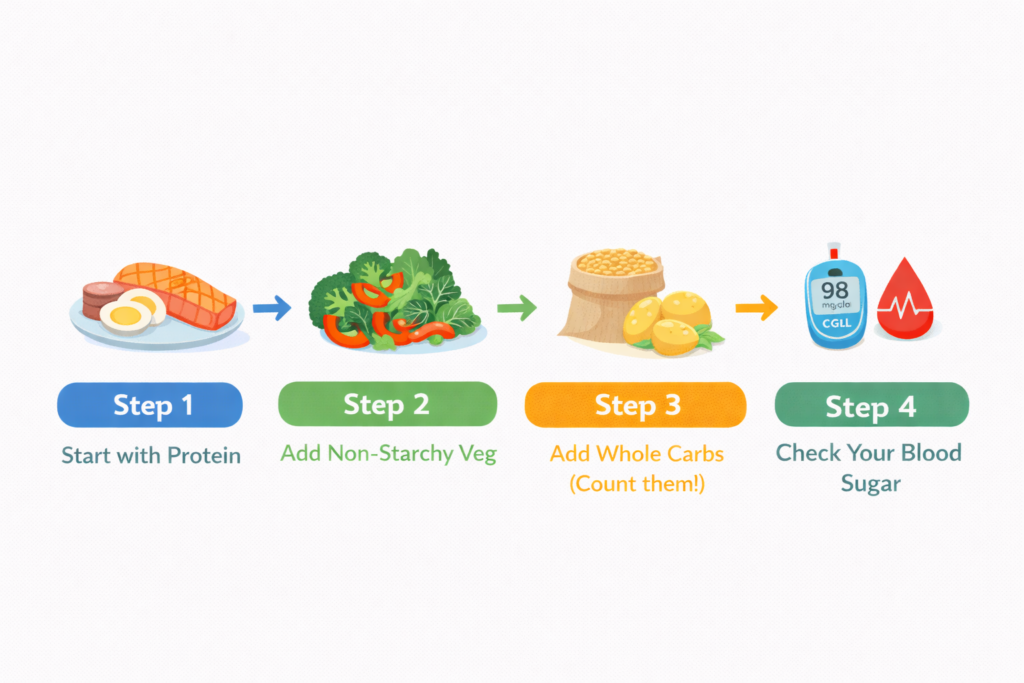
The satiety index is most useful as a practical guide when creating meals and snacks — not as a strict rule to follow. Here’s how to use it in everyday life:
 Step 1: Make protein the foundation of your meals
Step 1: Make protein the foundation of your meals
Protein is the most consistently filling macronutrient. Eggs, fish, chicken, tofu, Greek yogurt, cottage cheese, and legumes all provide protein and tend to enhance satiety. Start building each meal around a protein source before adding carbohydrate foods.
Step 2: Boost volume using non-starchy vegetables
Non-starchy vegetables — leafy greens, broccoli, cauliflower, cucumber, zucchini, peppers — have very low carbohydrate and high water content. They provide bulk and fiber without significantly increasing blood sugar levels. Goal: aim for at least half of your plate at lunch and dinner.
Step 3: Select whole carbohydrate foods instead of processed options
Whole fruit is more filling than juice. Steel-cut oats are more filling than instant oats. Whole-grain bread is more filling than white bread. Less processed carbohydrate foods also tend to raise blood sugar more gradually, making them better on the glycemic index.
Step 4: Combine carbohydrates with protein and/or healthy fat
Practical combinations that increase fullness and slow blood sugar spikes:
- Apple with peanut butter or almond butter
- Oatmeal with eggs or Greek yogurt with nuts
- Whole-grain toast with avocado and egg
- Brown rice or potatoes with fish or chicken and roasted vegetables
- Beans, vegetables, and a small amount of olive oil
Step 5: Use your glucose data to personalize it
Theory is helpful; your own data is better. After eating a meal you believe should be filling and blood-sugar-friendly, check what actually happens with your CGM or fingerstick readings. Over time, you’ll identify your personal ‘best bets’ — meals that keep you full, maintain stable blood sugar within your target range (typically 70–180 mg/dL / 3.9–10.0 mmol/L after meals), and suit your lifestyle.
Step 6: Adjust insulin or medication according to carbs, not satiety
If you take mealtime insulin or use an insulin pump, always dose based on the carbohydrate content of your meal and your personal correction factor — as agreed with your care team. A high satiety score does not reduce the carbohydrate content of food or your insulin need for it.
What does a diabetes-friendly, high-satiety meal plan entail?
These are practical meal ideas that offer high satiety and blood-sugar-friendly options. They are not prescriptions — work with your registered dietitian or certified diabetes care and education specialist (CDCES) to customize portions and timing.
Breakfast ideas
- Steel-cut oats topped with plain Greek yogurt, berries, and a handful of walnuts
- Two eggs scrambled with spinach and tomatoes, served with a small slice of whole-grain toast
- Cottage cheese topped with sliced peaches and a tablespoon of chia seeds
Lunch ideas
- Whole-grain wrap with tuna or grilled chicken, plenty of vegetables, and a piece of whole fruit
- Lentil and vegetable soup served with a small whole-grain roll
- Large salad with hard-boiled eggs, chickpeas, cucumber, olive oil, and a small serving of whole-grain crackers
Dinner ideas
- Baked salmon with roasted broccoli and a moderate serving of boiled or roasted potatoes (count carbs)
- Chicken stir-fry with mixed vegetables and a small serving of brown rice
- Bean and vegetable curry served over cauliflower rice or a small portion of whole-grain rice
 Snack ideas (if needed between meals)
Snack ideas (if needed between meals)
- Apple with 1–2 tablespoons of peanut butter
- A measured amount of plain air-popped popcorn (about 3 cups)
- Hummus served with sliced raw vegetables
- Cottage cheese with a small handful of berries
- A hard-boiled egg with several whole-grain crackers
How do satiety, glycemic index, and glycemic load interact?
For long-term patients who want to explore further, the most effective diabetes nutrition plan combines all three concepts together with your actual glucose data.
- Use the satiety index to select foods that satisfy hunger and prevent overeating.
- Use the glycemic index to choose foods that lead to slower, more gradual increases in blood sugar.
- Use glycemic load to better reflect the actual carbohydrate intake.
- Use your CGM or blood sugar readings to understand how your body responds — individual variation is important.
A food that performs well on all three — high satiety, low-to-moderate GI, manageable glycemic load — is a truly excellent choice for most people with diabetes. Think: legumes, non-starchy vegetables, eggs, fish, plain Greek yogurt, and most whole fruits.
Helpful Resources & Research
- ADA Standards of Care 2026: Section 5 — Facilitating Positive Health Behaviors and Well-being
- Holt SHA et al. A satiety index of common foods. European Journal of Clinical Nutrition. 1995. PMID: 7498104.
- Holt SHA et al. Interrelationships among postprandial satiety, glucose and insulin responses. European Journal of Clinical Nutrition. 1996. PMID: 8968699.
- Rakha A et al. Insights into the constellating drivers of satiety impacting human food intake. Comprehensive Reviews in Food Science and Food Safety. 2022.
- American Diabetes Association: Healthy Eating for Diabetes
- CDC: Diabetes Meal Planning
Frequently Asked Questions
What is the satiety index in relation to diabetes?
The satiety index rates how filling different foods are after equal-calorie servings compared to white bread (score = 100). For people with diabetes, it serves as a useful guide for selecting foods that curb hunger and reduce snacking — both of which help with weight management and maintaining stable blood sugar levels. It works best when combined with carb counting and your own glucose data, not as a substitute.
Which foods have the highest satiety ratings?
Boiled potatoes lead the list with 323 points, followed by fish (225), oatmeal (209), oranges (202), apples (197), and eggs (150). Foods high in protein and fiber tend to score the best. Remember that a high satiety score doesn’t mean a food is low in carbohydrates — potatoes, for instance, still need careful portioning for those with diabetes.
Does feeling full mean my blood sugar will be okay?
Not necessarily. A filling food can still significantly raise your blood sugar if it contains many carbohydrates. Boiled potatoes are one of the most filling foods tested, but they have a relatively high glycemic index. Always check your blood sugar (with a CGM or fingerstick) after meals to see how your body actually responds to different foods.
How does the satiety index differ from the glycemic index?
The satiety index shows how full a food makes you feel; the glycemic index shows how quickly it raises your blood sugar. A food can score high on one and not the other. For diabetes, the best foods usually score well on both — like fish, eggs, legumes, and whole fruits — but understanding the difference helps you make better choices.
Can I use the satiety index to lower insulin doses?
No. If you use insulin — whether through injections or an insulin pump — your dose should always be based on the carbohydrate amount in your meal and your personal settings, as advised by your care team. Feeling full does not lower the carbohydrates in food or your body’s need for insulin to process them.
Why do some filling foods still lead to blood sugar spikes?
Satiety and blood sugar response are controlled by different mechanisms. Boiled potatoes are very filling (satiety index 323), mostly because of a compound called protease inhibitor II, but they still break down into glucose. Pairing high-satiety carbohydrate foods with protein, fat, and non-starchy vegetables slows digestion and helps reduce blood sugar spikes after meals.
What are the best snacks for diabetes that also help you stay full?
A good snack options include an apple with peanut butter, cottage cheese with berries, hummus with raw vegetables, a hard-boiled egg with whole-grain crackers, or a small portion of air-popped popcorn. Each combines protein and/or fiber with moderate carbohydrates to promote fullness without a sharp rise in blood sugar. Your blood sugar target after a snack is generally under 180 mg/dL (10.0 mmol/L).
Do GLP-1 medications affectinfluence how the satiety index applies to me?
Yes. GLP-1 medicines like semaglutide (Ozempic, Wegovy) or tirzepatide (Mounjaro) slow stomach emptying and decrease appetite, which means you might feel full much sooner and require less food. The satiety index was developed in people not taking these medications. If you’re on a GLP-1 medicine, work with your care team on portion sizes and nutrition, as your hunger signals are already being altered.
Is the satiety index the same as the fullness factor?
They are similar but not exactly the same. The satiety index is based on Holt’s original research, which measured hunger over two hours in controlled settings. The ‘fullness factor’ is a related concept used in some nutrition tools to estimate satisfaction per calorie. Both focus on foods high in protein and fiber, but the satiety index has a stronger research basis for the scores mentioned in this article.
How can I begin incorporating the satiety index into my diabetes meal plan?
Start simple: at each meal, aim to include a high-protein food (fish, eggs, chicken, legumes), plenty of non-starchy vegetables, and a moderate portion of a whole-food carbohydrate. Use your CGM or blood sugar readings to track how different meals affect you. Over time, you’ll discover your personal ‘best bets’ — foods that keep you satisfied and maintain blood sugar within your target range of 70–180 mg/dL (3.9–10.0 mmol/L) after meals.
Last Updated on March 11, 2026

 How to Incorporate High-Satiety Foods into Diabetes Meal Planning
How to Incorporate High-Satiety Foods into Diabetes Meal Planning